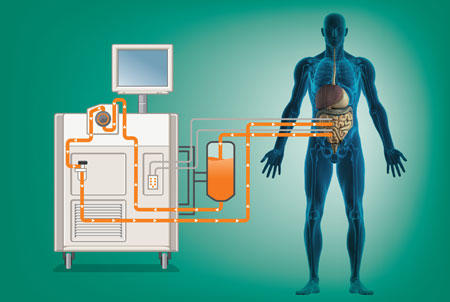
Hyperthermic intraperitoneal chemotherapy, or HIPEC, allows physicians to circulate very high concentrations of chemotherapy throughout the abdominal cavity with minimal to no exposure to the rest of the body.
Hyperthermic (or Heated) Intraperitoneal Chemotherapy (HIPEC) is a state-of-the-art procedure for treating cancers that have spread to the abdomen. In the past, patients with advanced cancers have had few medical alternatives. Today, HIPEC offers a new treatment option – even for people who have been told they have no options.
Froedtert Hospital in Milwaukee, Wis., is a leading cancer center for HIPEC surgery. Our physicians are active in HIPEC research and developing many HIPEC cancer treatment advances. Our Radiology Department is a leader in using advanced imaging technologies in the early detection of cancer, including cancers that can be treated with HIPEC.
HIPEC Video FAQ
Anai Kothari, MD, Ugwuji Maduekwe, MD, and Callisia Clarke, MD, surgical oncologists, explain heated intraperitoneal chemotherapy (HIPEC) in the video FAQ below.
What is HIPEC surgery?
HIPEC actually is a part of a typical surgical procedure that we offer for patients with advanced peritoneal-based disease, and it stands for heated intraperitoneal chemotherapy which basically describes what is happening during that portion of the operation. We will start by doing a major part of the procedure and then follow that up by infusing or perfusing a heated chemotherapy directly into the abdominal cavity. The goal of that is twofold. One, to help actually treat the tumor directly, and then also ensure that we're able to get adequate treatment directly at the peritoneal lining within the abdomen.
What diagnoses does HIPEC treat?
HIPEC is used in patients with advanced peritoneal disease or carcinomatosis. And that can be from several different causes of cancer and typically it's started in one place and has now spread to the peritoneal lining. Some of the most common things that it comes from is the appendix, the colon or the rectum, the ovaries or mesothelioma. There's a few other disease sites that actually can cause peritoneal involvement. Those are slightly more rare, but anytime we see a patient that has peritoneal involvement of the lining of their abdominal cavity with cancer, we think of HIPEC as one of the options for them.
What are the three phases of HIPEC surgery?
I usually break HIPEC surgery down into three phases. The first is cytoreduction and that really is focused on eliminating the tumor from within the abdominal cavity. There's a lot of procedures that may go into doing that, and that includes removing a portion of the bowel, potentially other organs - like the spleen or the gallbladder. So really, that first portion, the goal is to eradicate or remove all the tumor that we can visibly see.
The next portion is actually the heated chemotherapy portion and, again, that's really meant to directly put chemotherapy on the target organ so that we're directly treating the tumor where it actually is.
And then the last portion of the operation is you know, since the first part is taking out potential organs or structures, is restoring continuity or putting everything back together. It's an important part from a quality of life and long-term standpoint to do that part well, and so we focus a lot of time and energy on ensuring that is kind of the third part of the operation.
After the surgery, the recovery is an inpatient recovery. On average patients will stay in the hospital between 7 and 10 days. A lot of that is actually dependent on, not the chemotherapy itself, but what was necessary during the operation to clear the tumor. The chemotherapy, of course, adds some additional recovery time on top of just recovering from surgery itself. I usually advise patients that the short-term recovery takes about 6 weeks overall and sometimes the ramifications, the effects of the surgery, can last even longer than that. But the key is that this is part of a multidisciplinary approach to treating this cancer.
How would you describe outcomes for HIPEC?
Peritoneal surface malignancies are an interesting and varied group of disease processes. The way I think about the outcomes for HIPEC treatment is "Why are we doing the HIPEC treatment?" And I think for anyone who has a cancer that we're taking care of, our goals are ideally to prolong the length of life, but also to treat the disease and to improve symptoms.
How does HIPEC surgery benefit patients?
HIPEC is a really important part of the treatment paradigm or how we treat patients with a multidisciplinary approach for several different diseases. You know I emphasize that really when we think about treating patients with this advanced type of tumor, we have to think about not just the surgery itself, but kind of the medical treatment before and after. Sometimes that's in combination with things like radiotherapy or immunotherapy.
HIPEC is one part of kind of the larger focus of treatment for this disease. Where it's especially beneficial is that you know what we're offering is treatment that's directly at that site of disease, so the peritoneal cavity within the abdomen directly. And what that has an advantage over some of the other treatment modalities for this type of disease is that it's a directed therapy at the tumor at the site and so there's of course advantages to that over other therapies.
What clinical team members are part of the Froedtert & MCW HIPEC team?
We take a holistic approach to our patients with peritoneal surface malignancies here. And so from that stance, we think that the HIPEC team is not just people involved directly in giving the HIPEC, but everyone involved in managing these diseases to make sure that you have the best outcome. With that approach, I believe the HIPEC team includes our group of surgical oncologists, medical oncologists, radiation oncologists, our nutritionists, clinical psychologists, physical and medical rehabilitation team all working together to make sure patients get the best outcomes which results in improved life and improved quality of life.
Why is it important to choose an experienced HIPEC team for my surgery?
The biggest thing that a patient needs to take into consideration when undergoing HIPEC is the experience of the team that is providing their care. Studies have shown that your incidence of complication decreases significantly when you have your surgery at centers that are more experienced. We are proud to have taken care of hundreds of patients with peritoneal surface malignancies. Because we are a regional high volume center, our complication rates are much lower than national averages.
What are benefits of receiving HIPEC at the Froedtert & MCW Cancer Network?
We have decades of experience taking care of patients with peritoneal surface malignancies and implementing HIPEC as one of the elements of the treatment of those patients. One of the benefits that has accrued to us taking care of these patients is not only are they exposed to everyone across the institution being used to the care of these patients from the nurses to the radiologists to the nutritionists. We also have a very longstanding and expert multidisciplinary tumor board at which every patient we see here who has a peritoneal surface malignancy and is eligible for HIPEC treatment is seen and evaluated, so not only do all those team members interact with patients but they're all we sit down and discuss their entire plan and review their pathology with everyone. That is one of the benefits of of receiving care at an institution like this.
HIPEC Procedure Uses Cytoreductive Surgery and Chemotherapy
“Intraperitoneal” means within the peritoneum, which is a membrane that lines the abdominal cavity. There are two parts to the HIPEC procedure:
A Delavan woman was shocked to learn she had 30 pounds of tumors growing in her stomach from a rare type of appendix cancer. Her cancer team performed a HIPEC procedure to the abdomen. Now, six months later, the patient is cancer free and spreading the word about the outstanding care she received. Watch her story >>
- Cytoreductive surgery
- At the start of the HIPEC procedure, a surgeon uses a minimally invasive scope called a laparoscope to inspect the inside of a patient’s abdomen.
- If existing cancer tissue can be removed completely, a surgical incision is created.
- The surgeon then works systematically throughout the abdomen to remove all visible tumors.
- Tumor tissue can be removed using several methods, including ultrasonic ablation, thermal ablation (electroevaporative surgery, microwave) and cryoablation (or freezing).
- Chemoperfusion
- After all visible cancer tissue has been removed, the surgical team circulates a concentrated chemotherapy solution throughout the abdomen. The purpose is to expose microscopic cancer cells to the cancer-killing drug.
- The chemotherapy solution is heated to approximately 102 degrees Fahrenheit, which increases the anti-cancer effect. This part of the procedure was sometimes referred to as a "hot chemotherapy," “hot chemo bath” or "chemo wash."
- The surgical team circulates the solution for approximately 90 minutes, delivering high-dose chemotherapy to cells that coat the lining of the abdomen.
- Afterward, the abdomen is washed with a sterile solution.
The entire HIPEC procedure takes from six to eight hours.
HIPEC Resources
HIPEC Treatment Benefits
HIPEC offers several treatment benefits for patients with cancers that have spread to the abdomen:
- Higher drug concentration. With standard intravenous chemotherapy, cancer drugs are delivered throughout the body, affecting cancerous tumor and healthy tissues. This limits the dose that can be delivered safely. In the HIPEC procedure, cancer drugs are confined to the abdomen. This allows physicians to deliver cancer drugs at a much higher concentration, increasing the chemotherapy’s effectiveness.
- Greater contact with cancer cells. Abdominal tumors usually have a very poor blood supply, so standard chemotherapy delivered through the bloodstream does not reach these tumors easily. HIPEC directly exposes abdominal tumors to anti-cancer drugs.
- Greater tissue penetration. The high temperature of the HIPEC solution causes tiny blood vessels in the abdomen to dilate. This allows the drug to penetrate abdominal tissues more deeply, exposing more microscopic cancer cells to chemotherapy.
- Better targeting of cancer cells. Heat also speeds up the cancer cell cycle, which makes cancer-targeting drugs work even better.
- Fewer side effects. HIPEC confines chemotherapy to the abdomen, with very little delivery of drug to the rest of the body. Patients experience fewer HIPEC side effects than can be associated with chemotherapy.
- Reduced hospital stay. Our physicians have pioneered short stay recovery programs. Through careful anesthesia management and advanced surgical techniques, we have virtually eliminated an intensive care unit (ICU) stay after HIPEC, which is common in many centers worldwide. Patients typically stay in the hospital for about five to 10 days after this operation.
- Minimally invasive operation for eligible patients: Our physicians have developed significant expertise in the technique of laparoscopic HIPEC. This technique is available to patients with early cancers and to patients needing HIPEC for control of ascites fluid in the abdomen.
HIPEC Treatment Outcomes
HIPEC has led to dramatic improvements in outcomes for patients who have challenging cancer diagnoses.
- Increased survival. Studies show that HIPEC significantly increases survival for patients with cancers that have spread to the abdomen. In fact, HIPEC has achieved long-term cures for some patients.
- Cancer as a chronic disease. When a cure is not possible, HIPEC allows physicians to treat cancer less like a terminal condition and more like a chronic disease such as diabetes or high blood pressure. Even as the cancer progresses, physicians can often use HIPEC and other therapies to control the disease and its symptoms.
- Ascites control. Cancers that have spread to the abdomen sometimes cause ascites, which is the buildup of fluid within the peritoneal cavity. This fluid accumulation can lead to swelling of the abdomen, discomfort, pain, difficulty breathing and organ failure. HIPEC is very effective at controlling ascites related to the spread of cancer.
- Low complication rates. Care teams that treat a high number of HIPEC patients have low complication rates. Froedtert Hospital is one of the busier HIPEC centers in the nation, and our HIPEC surgeons’ complication rates are lower than national averages.
- Improved quality of life. Research has shown that HIPEC can help patients maintain their overall quality of life, with significant reductions in pain and distinct gains in emotional health.
- Prevention of bowel obstruction. Patients with advanced abdominal cancers may develop bowel obstructions that can prevent them from being able to eat. Initiated early, HIPEC can prevent bowel obstructions. The HIPEC team also has advanced expertise in the management of patients with bowel obstructions.
Who Is a Candidate for HIPEC?
HIPEC can be used to treat cancers that have spread to the abdomen and several cancer-related conditions:
- Abdominal cancer, gastric cancer, and cancer-related conditions, including peritoneal cancer such as peritoneal mesothelioma, pseudomyxoma peritonei (PMP) and primary peritoneal carcinomatosis
- Appendix cancer
- Colorectal cancer/colon cancer
- Gallbladder cancer
- Ovarian cancer
- Pancreatic cancer
- Sarcomas, including GIST tumors and desmoplastic small round cell tumors (DSRCTs)
- Stomach cancer (gastric cancer)
- Thoracic mesothelioma
Based on imaging and/or diagnostic laparoscopy, as well as the disease pathology, we decide if the patient is a candidate for cytoreductive surgery (debulking the tumor). In some cases, we may start with systemic chemotherapy to reduce the tumor size and follow up with tumor debulking and HIPEC targeted specifically to where the disease is in the body.
HIPEC can also be used as a preventive treatment for patients with cancers at high risk of spreading to the abdomen. Our physicians have pioneered the use of diffusion-weighted MRI technology to detect metastatic abdominal tumors. Early detection of metastatic disease and prompt treatment significantly extend survival for people with these cancers.
HIPEC can be performed safely for a wide range of patients, including elderly people, people who have had previous cancer treatments and patients with other health conditions.
Some patients are initially ineligible for HIPEC because their cancer is too extensive for surgical removal. For many of these patients, targeted chemotherapy initiated by medical oncologists can often shrink their tumors enough to make them candidates for the procedure.
HIPEC Risks
Procedure risks can vary based on the extent of surgery that is performed. Some of the risks include infection, bleeding, blood clots, hernia, leakage, damage to adjacent organs and/or blood vessels, ileus, alterations to blood counts and changes to hair and nails.
The HIPEC Patient Experience at Froedtert Hospital in Milwaukee
We put patients and their families at the center of HIPEC treatment. Our care pathway has been carefully designed to ensure a smooth treatment journey and the best possible outcomes.
Care navigators. With our patient-centered care model, patients who might be candidates for HIPEC work directly with a new patient coordinator. The coordinator will introduce you to the program, gather your medical records and schedule a physician consultation. An advanced practice provider will review your medical records and coordinate additional appointments. Our goal is to “cluster” appointments for the convenience of patients, especially for individuals and family members traveling to Froedtert Hospital from a distance.
First visit. During your first visit, you will meet with a HIPEC surgeon and other cancer specialists. We will review your history, as well as your imaging results, and discuss the options. A plan will be formulated with clear steps outlined that could consist of chemotherapy, additional testing or surgery scheduling. If HIPEC is right for you, your physician will talk to you about the procedure, discuss the risks and benefits, and explain the recovery process. Your involvement in decision making helps us tailor a treatment plan to your specific needs and concerns. During your first visit, you will also meet with specially trained cancer nurses, cancer dietitians, counselors and physical therapists.

“Everyone I met was focused on me, the patient. They created such a positive atmosphere." Ann Starr, appendix cancer survivor
Support services. Our “HIPEC Buddy” program gives you the opportunity with talk to another patient who has previously undergone the HIPEC procedure. Your buddy is available to answer your questions about HIPEC, help you understand what to expect and talk through your concerns. Our team will also help you address your personal, financial and family issues through the many support services available in our Jeffrey C. Siegel Quality of Life Center.
Cancer and nutrition. Cancer and its treatment can affect the body’s ability to heal, to absorb nutrients, tolerate specific foods and maintain a healthy weight. A registered dietitian meets with patients before and after surgery to evaluate their nutritional status and develop a long-term plan to ensure that calorie and protein needs are met. This is an important step in laying the groundwork for optimal recovery. After surgery, nutritional needs will change and some patients need special nutritional support and instruction. Our registered dietitians can also help patients manage side effects and provide guidance on appropriate and helpful supplements such as vitamins and minerals.
“Prehab to Rehab.” Preparation for a successful recovery begins before surgery. HIPEC team therapists will begin by assessing your functional abilities. They will then work with you to create a home exercise program to build your upper body, lower body and core strength. Exercise plans typically include a walking or biking program to increase endurance. You will also work with a specialized cancer dietitian to help ensure you go into surgery with a strong nutritional foundation and peak immune system function.
Recovery and return home. After surgery, you will spend seven to 10 days in the hospital and be cared for by nurses and others with special training in the needs of HIPEC recovery patients. Most patients do not require an intensive care unit stay. Advanced practice providers, occupational therapists, dietitians, and others will help you achieve a strong recovery and an early return to normal life. At home, you and your family will have immediate phone access to an oncology nurse to address any issues that arise. Most patients resume their regular daily activities, but you may be fatigued and you may need to adjust to changes in your bowel function. An occupational therapist will re-assess your functional ability and adjust your exercise program as needed. In addition to scheduled follow-up appointments, you will have regular contact with your care team via phone, e-mail and MyChart. It could take roughly three to six months to return to your baseline quality of life.
For patients traveling from a distance. Many people, including international patients travel long distances to seek HIPEC treatment at Froedtert Hospital. We are located just 30 minutes from Milwaukee’s General Mitchell International Airport and are about 90 miles north of Chicago and O’Hare International Airport with convenient proximity to major highways, nearby hotels and other amenities for travelers. Learn more about services at the hospital and nearby community.
No matter where patients live, our HIPEC team’s goal is to make your time with us and your return home a positive experience. We’re happy to collaborate with a patient’s own physician to transition care and make sure recovery and ongoing treatment needs are well-coordinated.
HIPEC Surgeons and Program Staff
HIPEC is an advanced therapy that requires strong multidisciplinary care. Our team members work together to provide fully personalized care plans and support services to ensure a good care experience and the best medical outcome.
Our HIPEC team is led by surgical oncologists who are national leaders in HIPEC treatment and research. The HIPEC team also includes medical oncologists, radiation oncologists, dedicated nurses, advanced practice providers, cancer dietitians, physical therapists, occupational therapists, care coordinators, specially trained surgery staff and other specially trained providers.
HIPEC Surgeons
T. Clark Gamblin, MD, MS, MBA
Alexandra C. Istl, MD, MPH, FRCSC
Anai N. Kothari, MD, MS
Ugwuji Maduekwe, MD, MMSc, MPH, FACS
Dave Lal, MD, MPH (Pediatrics)
HIPEC Oncologists
Ben George, MD
James P. Thomas, MD, PhD
HIPEC Advanced Practice Providers
Lisa Graber, APNP
Jennifer Merrill, NP
Tanya Radke, APNP
HIPEC Dietitian and Integrative Dietary Counselor
Julia Thompson, MS, RD, CD, CNSC
HIPEC Physical Therapist
Chris Walczak, PT
Affiliated Faculty
Colorectal Surgery
Kirk Ludwig, MD, FACS, FACRS
Carrie Peterson, MD
Timothy Ridolfi, MD
Gynecologic Oncology
William Bradley, MD, FACOG
Denise Uyar, MD, FACOG
Erin Bishop, MD, FACOG
Janet Rader, MD, FACOG
Radiation Oncology
Beth Erickson, MD
William Hall, MD
Radiology
Charles Marn, MD
Naveen Kulkarni, MD
Vascular and Interventional Radiology
Sarah White, MD, MS
Eric Hohenwalter, MD, FSIR
Parag Patel, MD, MS
Robert Hieb, MD, RVT, FSIR
William Rilling, MD, FSIR
Clinical Trials
Our specialists are involved in clinical trials for many different types of cancer, including cancers that may be treated by HIPEC, offering eligible patients access to new treatment concepts.
