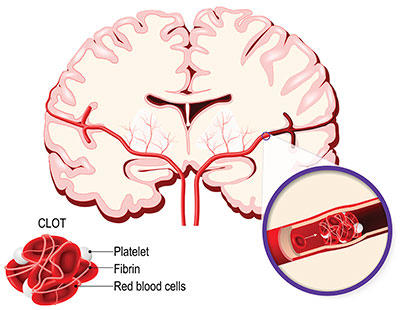
Your brain needs a constant supply of oxygen. From the moment you see stroke symptoms, every minute makes a difference.
Remember BE FAST
- Balance. Sudden loss of coordination or balance.
- Eyes. Sudden change in vision.
- Face. Weakness on one side or facial droop.
- Arm or leg. Weakness or numbness.
- Speech difficulty. Slurred or trouble understanding speech.
- Terrible headache. Sudden onset.
If you have sudden onset of any of these symptoms, call 911 right away!
Reduce Your Stroke Risk
Did you know 80% of strokes could be prevented? You can reduce your risk of stroke by taking these steps.
- Control your blood pressure, cholesterol and blood sugars.
- Avoid smoking.
- Eat a healthy diet.
- Exercise.
Video developed in partnership between high school students from Elmbrook and Wauwatosa in the health care segment of the LAUNCH Program and mentors from the Froedtert & MCW stroke team. The group received an award from the Coverdell Stroke Program, part of the Wisconsin Chronic Disease Prevention Program (CDPP).
When Seconds Count for Stroke Survival and Recovery
Acute Stroke Team Available 24/7 at Froedtert Hospital
Seconds count when responding to a stroke. Neurons die rapidly during the first hours after stroke onset, and limiting the extent of damage requires urgent diagnosis and treatment.
The Froedtert Acute Stroke Team is ready 24 hours a day to respond to the acute needs of stroke patients. Members have the training and expertise to treat all types of stroke safely and efficiently and a neurologist is available onsite around the clock.
Acute Stroke Team Facts
Our stroke experts offer patients the following advantages:
- 24/7 emergency department coverage by stroke specialists
- Specialized protocols for rapid evaluation
- Average door-to-CT (diagnosis) time less than 30 minutes
- Average door-to-needle (clot-busting medication) time less than 40 minutes
- More procedures for stroke intervention are performed at Froedtert Hospital than any other hospital in Wisconsin.
Certified by The Joint Commission
The Joint Commission recognizes Froedtert Hospital as a Comprehensive Stroke Center. They have also recognized Froedtert Menomonee Falls Hospital and Froedtert West Bend Hospital as Primary Stroke Centers. These certifications demonstrate our commitment to providing you or someone you love with the best care in the event of a stroke. Learn more about The Joint Commission certifications.

Team members include critical care neurologists, interventional neurologists, neurosurgeons, emergency medicine physicians and nurse specialists – all of the experts needed for complete emergency stroke care.
As eastern Wisconsin’s only certified Adult Level I Trauma Center, physicians and staff at our Emergency Department are specially trained in stroke recognition. They also are experts in emergency treatment for ruptured brain aneurysms and raised intracranial pressure, an increase in pressure inside the skull that results from or causes brain injury.
We treat stroke at the following locations:
- Froedtert Hospital, Comprehensive Stroke Center, Milwaukee
- Froedtert Menomonee Falls Hospital, Primary Stroke Center, Menomonee Falls
- Froedtert West Bend Hospital, Primary Stroke Center, West Bend
We collaborate with Flight For Life for emergency air transport and work with hospitals throughout the area to transfer patients or bring physician expertise to them.
Stroke Resource Group on Facebook
This page is open to the community, stroke survivors, family members, caregivers and health care staff with a focus on resources. It is in no way a platform for medical advice. We look forward to interacting with new members and are always looking for ideas to improve our outreach to the community.

Recognized as High Performing by U.S. News & World Report
Froedtert Hospital and Froedtert Menomonee Falls Hospital are recognized by U.S. News & World Report as high performing in stroke care.More to Explore