Abdominal aortic aneurysm (AAA) occurs in the part of the aorta that passes through the abdomen. Men are more likely to develop abdominal aortic aneurysms than women, and the risk increases with age. Our specialists, including vascular surgeons, vascular medicine specialist and vascular and interventional radiologists, have extensive experience diagnosing and treating all types of aortic aneurysm.
Waterford man grateful to be alive after ruptured aneurysm
Walter Foster was rushed to Froedtert Hospital after his AAA burst while he was in a local emergency room being treated for pain that he thought was kidney stones. Peter Rossi, MD, and his team operated for two and a half hours to repair the rupture. Dr. Rossi noted that about 90% of people with an AAA rupture do not make it to the hospital and emphasized the importance of screening if you are at risk. Read the story from the Racine Journal Times.
Risk Factors
Several factors can increase the risk of developing an abdominal aortic aneurysm.
- Smoking
- Family History of AAA
- Atherosclerosis (hardening of the arteries)
- Peripheral Artery Disease (PAD)
- High cholesterol
- High blood pressure
- Marfan Syndrome
- Other connective tissue disorders
Men over the age of 65 with a history of smoking or a history of atherosclerosis are at the highest risk for developing AAA.
Symptoms
Most abdominal aortic aneurysms are detected without any symptoms present, often through a routine physical exam, or X-ray or CT or imaging for an unrelated condition. Other symptoms may include a pain in the abdomen or lower back that may radiate to the groin or legs or the feeling of pulse in the abdomen. A ruptured aneurysm requires emergency treatment and usually produces sudden symptoms including severe back or abdominal pain, nausea and vomiting, loss of consciousness or shock.
Treatments
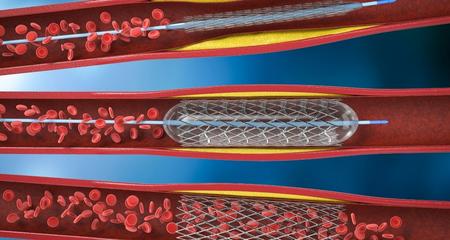
Abdominal aortic aneurysms can be treated different ways, depending on several factors, including the size, shape and location of the aneurysm, and the age and overall condition of the patient. Each approach has risks and benefits, and patients should understand all of their options to make an informed decision. Options include open surgery, minimally invasive endovascular procedures or no procedure.
- Close monitoring – Small abdominal aneurysms may not require immediate repair. Regular follow-up exams are necessary to monitor the aneurysm for any changes or signs that repair is needed.
- Endovascular aneurysm repair (EVAR) (minimally invasive)
- Open surgical aneurysm repair
Recognized as High Performing by U.S. News & World Report
Froedtert Hospital is recognized by U.S. News & World Report as high performing in three adult specialties and 16 procedures and conditions, including abdominal aortic aneurysm repair.Virtual Visits Are Available
Safe and convenient virtual visits by video let you get the care you need via a mobile device, tablet or computer wherever you are. We'll assess your condition and develop a treatment plan right away. To schedule a virtual visit, call 414-777-7700.
More to Explore