Lyme disease is the most common tick-borne disease in the United States with about 476,000 cases diagnosed and treated. In the Midwest, tick-borne diseases are on the rise as milder winters have made "tick season" an almost year-round event.
What Is Lyme Disease?
Lyme disease is a bacterial infection caused by Borrelia burgdorferi and possibly Borrelia mayonii, a newly discovered bacteria similar to Borrelia burgdorferi. You get Lyme disease when you come into contact with the bacteria through a tick bite.
When an infected tick bites the skin, bacteria enter where the tick is feeding. It takes at least 24 hours for Lyme disease bacteria to transmit because the bacteria need to change their own gene expression to infect an animal. There are other pathogens that can be transmitted in a matter of hours. In general, the longer a tick is attached, the higher the risk of infection.
Do All Ticks Transmit Lyme Disease?
In Wisconsin, there are at least 16 species of tick, but not all of them transmit disease to humans. Only one type of tick, Ixodes scapularis (commonly known as the black-legged tick or deer tick), carries and transmits Lyme disease. Contrary to what the tick’s name might imply, deer do not transmit Lyme disease bacteria to ticks. Deer are simply a common food source for the ticks. Also, not all of the Ixodes scapularis ticks are capable of transmitting Lyme disease. Only those that carry the bacteria can transmit it.
Other Tick-Borne Diseases on the Rise
There are five different types of infections that can be transmitted by the bite of the Ixodes scapularis tick – Powassan virus, anaplasmosis, ehrlichiosis, babesiosis and Lyme disease. While Lyme disease is the most prevalent, these other diseases are catching up.
Lyme Disease Protection
Taking steps to protect yourself and your family from ticks is the best way to ensure you stay healthy. While peak tick season is when ticks are most active particularly from May to September, the risk still exists from October to April, especially when temperatures are warmer.

Ticks should be removed as soon as possible per the CDC’s recommendations, with tweezers and by pulling upward with steady pressure. Tick removal tools (a plastic or metal v-shaped notch) and kits are widely available online and in some health care locations.
Conduct a thorough tick check and examine clothing, hair and skin after spending time in grassy or forested areas. A close examination is important, as juvenile ticks can be the size of a poppy seed or smaller. Look for a tiny, shiny freckle. If you find a tick, remove it carefully, take a picture and save it in a bottle or sealable plastic bag, as it could provide helpful information.
There are online resources that can help identify the most common ticks. If the tick you pulled off is not a black-legged tick, you do not have to worry about Lyme disease. Keeping the tick in a plastic bag can help you identify it by comparing it to photos online. For example, the very common dog ticks and wood ticks look quite different.
If you think you have a tick bite, talk to your primary care provider as soon as possible.
-
Ways to Prevent a Tick Bite
-
Use insect repellent containing at least 20% diethyltoluamide (commonly known as DEET). Lemon eucalyptus oil is also an effective option to repel ticks. Consult EPA.gov to read more about which repellent is best for you.
Use permethrin (an anti-parasitic product) to treat clothes, shoes, camping or hunting gear. Do not apply permethrin on skin.
Wear clothing that you can tuck into pants and socks to prevent ticks from getting on the skin. Light-colored clothing also helps you spot ticks easily.
Stay in the center of hiking trails and avoid areas with high grass and brush.
After being outside, do a full-body check, including in and around hair and clothes.
Check pets and any outdoor gear, as they can carry ticks into the house that can attach to a person.
Shower as soon as possible after time outdoors.
Lyme Disease Symptoms

Early symptoms of Lyme disease can appear anywhere between three and 30 days after a tick bite, and they can often mimic symptoms of other diseases. It is important to talk to your health care provider about your symptoms and if you think you may have had a tick bite.
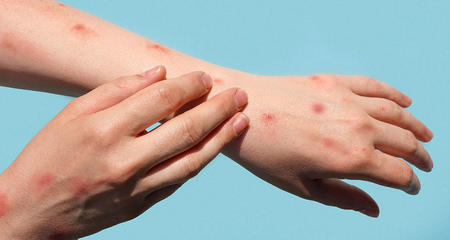
A classic early sign that an individual has been infected with Lyme disease is erythema migrans, a rash that begins at the site of the tick bite and gradually increases in size. It won’t be painful or itchy. It will look like a red spot that is at least two and a half inches in diameter and expands day to day.
Early Lyme Disease Signs and Symptoms
- Rash development — erythema migrans
- Flu-like symptoms that may include fever and chills
- Enlarged or swollen lymph nodes
- Muscle and joint aches
- Fatigue
Later Lyme Disease Signs and Symptoms in Untreated Individuals
- Severe headaches
- Facial palsy (drooping on one or both sides of the face)
- Increased muscle and joint pain
- Memory loss
- Numbness or tingling due to nerve problems
- Irregular heartbeat, known as Lyme carditis
Detecting Lyme Disease With Laboratory Tests
Lyme disease diagnosis relies on clinical observations and laboratory tests for the presence of antibodies against the B. burgdorferi bacteria. Since it can take several weeks for antibodies to develop against the bacteria, lab tests help confirm the diagnosis. If Lyme disease goes undetected and untreated, the disease will continue to progress and symptoms may appear months after the tick bite. Some patients who have untreated Lyme disease are hospitalized because the bacteria can affect the brain, the nervous system and the heart.
The CDC recommends a two-step laboratory blood sample test to accurately diagnose Lyme disease. New tests are also being developed as alternatives to the two-step process but still require review and clearance from the Food and Drug Administration.
It is not always necessary to obtain a blood test to confirm early Lyme disease since the necessary protein antibodies in the blood that make a test positive may take many days to form. Thus, it is common to have a negative blood test early in infection. If a patient is at risk and might have an infection early, it is usually better to treat for Lyme disease rather than rely on a blood test. Blood tests are more helpful for late disease that may have gone untreated early in the infection course.
Lyme Disease Treatment
Lyme disease can be very serious if left untreated. Treatment as soon as symptoms appear is important to prevent complications from the disease. Lyme disease has three stages with different levels of treatment.
- In most early-stage cases, Lyme disease has not spread throughout the body. It can be treated with oral antibiotics for a period of two to three weeks, and the patient can make a full recovery.
- As the bacteria begin to spread throughout the body, it becomes increasingly difficult to fight Lyme disease, though it is still treatable with antibiotics.
- In more advanced cases, the bacteria have spread throughout body. When this happens, hospitalization and intravenous antibiotics may be necessary.
Post-Treatment Lyme Disease Syndrome
Post-treatment Lyme disease syndrome (PTLDS) occurs when a person who was infected with Lyme disease and who was appropriately treated with oral antibiotics continues to experience symptoms. It is still unclear what causes PTLDS, and it is an important area of research for Lyme disease experts. Approximately 10% of people who were treated for Lyme disease have persistent symptoms that last for more than six months. PTLDS is sometimes referred to as chronic Lyme, but this term is outdated and is no longer used by experts in Lyme disease research or clinical care.
Symptoms of PTLDS include:
- Joint pain (stiffness, inflammation or swelling)
- Muscle pain
- Headache
- Severe fatigue
- Difficulty sleeping
- Cognitive impairment
- Memory problems
PTLDS is diagnosed based on a history of a Lyme disease infection documented through testing and treatment with appropriate antibiotics. When the symptoms persist, the patient may be diagnosed with PTLDS. For patients with chronic symptoms whose Lyme disease testing is negative, further testing for other disorders should be offered so the right diagnosis can be reached and appropriate therapy can be prescribed. Specific tests depend on the symptoms.
There is no proven treatment for PTLDS. Patients with PTLDS should seek treatment from a multidisciplinary team that can address their unique constellation of symptoms. Patients with PTLDS are occasionally treated with medications to reduce the inflammation that may persist after the bacteria are gone. Other PTLDS treatment recommendations can include physical and occupational therapy, as well as other supportive therapy to help with recovery from the physical and mental damage caused by the illness. In some cases, some symptoms of PTLDS may disappear over time without further treatment.
Similarities and Differences Between COVID-19 and PTLDS
Both PTLDS and COVID-19 can cause fatigue, but what causes it is not well understood yet. It is important to recognize that COVID-19 has a relatively high mortality rate in infected individuals as compared to many other infectious diseases, but no form of Lyme disease has a high mortality rate. In addition, there are many antibiotic therapies that are effective against Lyme disease and other bacterial infections, but there are fewer therapies available for COVID-19 and other viral infections. With either a COVID-19 infection or a Lyme disease infection, it is important to remember that medication will not repair already existing tissue damage caused by the infection. Antivirals for COVID-19 or antibiotics for Lyme disease are instead effective in stopping the infection from progressing.